Bile Reflux Gastritis Treatment in Daly City, CA
Bile reflux gastritis occurs when bile, a digestive fluid produced by your liver, flows backward from your small intestine into your stomach and esophagus. This backflow causes inflammation, pain, and damage to the stomach lining.
Unlike acid reflux, bile reflux involves alkaline digestive juices that standard acid-reducing medications can’t effectively treat.
At Center for Diabetes and Cardiometabolic Health (CDCH) in Daly City, our gastroenterology specialists provide comprehensive diagnosis and treatment for bile reflux gastritis and related bile disorders.
What Causes Bile Reflux Gastritis?
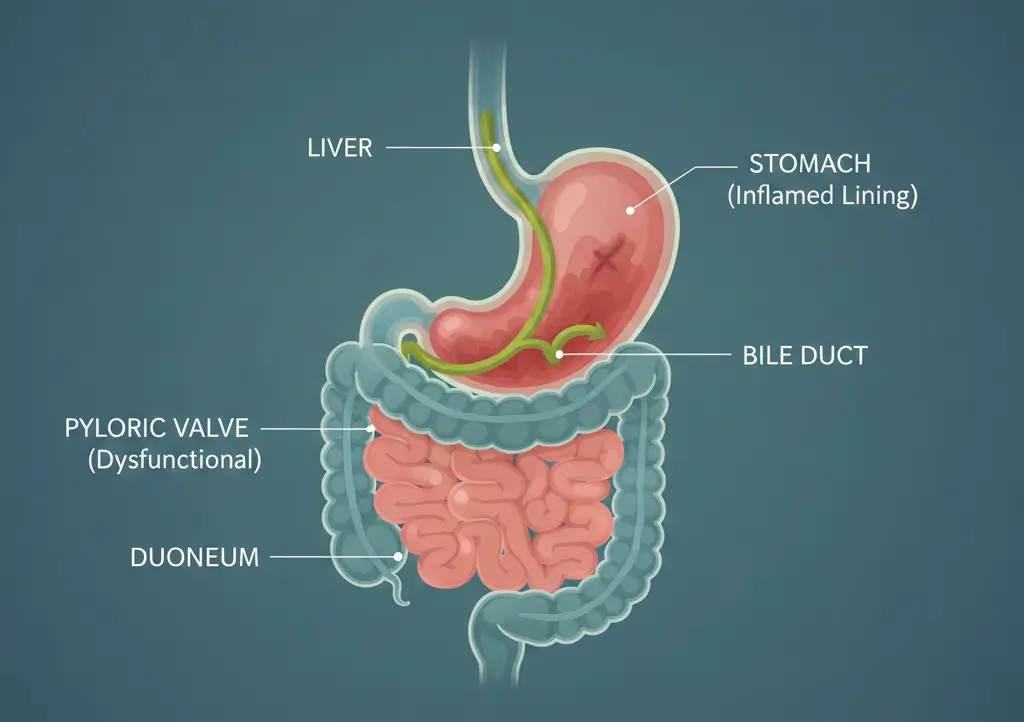
Bile reflux happens when the pyloric valve—the muscular ring between your stomach and small intestine—doesn’t function properly. This pyloric valve dysfunction allows bile to flow backward from the duodenum into the stomach.
This duodenogastric backflow brings bile acids and pancreatic enzymes that irritate and inflame the stomach lining, causing mucosal inflammation and damage.
Common Risk Factors
Cholecystectomy
Gallbladder removal causes continuous bile flow, which increases reflux risk.
Gastric bypass surgery
Alters normal anatomy and disrupts the pyloric valve function
Peptic ulcers
Can damage the pyloric sphincter.
Diabetes
Causes gastroparesis (delayed stomach emptying), which increases bile reflux likelihood.
Understanding your specific risk factors helps us create targeted treatment plans.
Bile Reflux vs Acid Reflux: Key Differences
Acid Reflux (GERD)
- Stomach acid flows into esophagus
- Burning sensation in chest
- Responds to antacids and PPIs
- Caused by lower esophageal sphincter weakness
- More common condition
- Dietary triggers: spicy, fatty, acidic foods
Bile Reflux
- Bile flows from small intestine to stomach/esophagus
- Upper abdominal pain, nausea
- Doesn't respond well to acid reducers
- Caused by pyloric valve dysfunction
- Often occurs after gallbladder surgery
- Bile is alkaline, not acidic
- Many patients have both conditions simultaneously, requiring different treatment approaches.
Common Bile Reflux Symptoms We Treat
Upper abdominal pain (burning or gnawing discomfort)
Bile vomiting (yellow-green colored vomit)
Persistent nausea
Heartburn that doesn't respond to acid reducers
Hoarseness or chronic cough
Unintentional weight loss
Bilious taste in mouth
Frequent burping
Feeling full after eating small amounts
Symptoms of bile reflux disease often worsen after meals, especially fatty foods.
Our Bile Reflux Diagnosis Process
Comprehensive Medical History
We review your symptoms, previous surgeries (especially gallbladder removal), medications, and risk factors for bile reflux
Upper Endoscopy (EGD)
Visual examination of your esophagus, stomach, and duodenum. Bile in stomach endoscopy appears as yellow-green fluid and gastric inflammation. We take biopsies to assess mucosal damage and rule out Barrett's esophagus or cancer
Advanced Diagnostic Testing
HIDA scan (hepatobiliary scintigraphy) measures bile flow and gallbladder function. Bilitec monitoring tracks bile exposure in the esophagus over 24 hours. Esophageal impedance-pH testing distinguishes between acid and non-acid reflux
Assessment of Complications
Testing for Barrett's esophagus, esophagitis severity, peptic ulcers, and gastric cancer risk
- Accurate diagnosis is essential because bile reflux requires different treatment than standard acid reflux.
Comprehensive Management for Bile Reflux
Combining medical treatments and lifestyle strategies for holistic care.
Bile Acid Sequestrants
Medications like cholestyramine and ursodeoxycholic acid (UDCA) bind bile acids in the stomach, reducing irritation and inflammation. These are the primary medical treatments for bile reflux gastritis. Cholestyramine comes as a powder mixed with water or juice, taken before meals. UDCA is available in tablet form and also helps dissolve cholesterol gallstones.
Prokinetic Agents
These medications improve stomach emptying and strengthen the pyloric valve, reducing bile backflow. Prokinetics help restore normal digestive motility.
Other Medications
Proton pump inhibitors (PPIs) may be prescribed if you have concurrent acid reflux, though they don't treat bile reflux directly. Sucralfate coats and protects the stomach lining from bile damage.
Addressing Underlying Causes
If diabetes-related gastroparesis contributes to bile reflux, improving blood sugar control is essential. Treating peptic ulcers that damage the pyloric sphincter helps restore normal function. In severe cases where medications fail, surgical interventions may be considered to redirect bile flow away from the stomach.
Low-Fat Diet
Bile is released in response to dietary fat. Reducing fat intake decreases bile production and reflux. Focus on lean proteins, whole grains, fruits, and vegetables. Avoid fried foods, fatty meats, full-fat dairy, and rich desserts.
Meal Frequency
Eating smaller portions more frequently throughout the day prevents excessive stomach distension, reducing the likelihood of backflow through the pyloric valve.
Meal Timing
Strategic timing of meals is crucial; specifically, avoiding intake close to bedtime ensures that gravity assists in keeping bile in the small intestine.
Triggers
Certain dietary triggers can exacerbate symptoms; identifying and removing these personal triggers is a core component of symptom management.
Wellness
Maintaining a healthy weight reduces abdominal pressure that contributes to reflux. Stress management through meditation, yoga, or counseling helps—stress affects digestive function and can worsen bile reflux symptoms.
Preventing Serious Complications
Untreated bile reflux gastritis can lead to significant health problems. Chronic bile exposure damages the esophageal lining, causing esophagitis and potentially Barrett’s esophagus—a precancerous condition. Long-term gastric inflammation increases gastric cancer risk. Bile reflux can cause or worsen peptic ulcers in the stomach and duodenum. Early diagnosis and treatment prevent these serious complications.
Bile Reflux After Gallbladder Surgery
Bile acid reflux gastritis is particularly common after cholecystectomy (gallbladder removal). Without the gallbladder to store and regulate bile release, bile flows continuously into the small intestine.
This continuous flow increases the likelihood of bile refluxing backward into the stomach, especially if the pyloric valve doesn’t function optimally.
If you’ve had your gallbladder removed and are experiencing persistent upper abdominal pain, nausea, or bile vomiting, you may have post-cholecystectomy bile reflux.
Treatment After Gallbladder Surgery
Combining medical treatments and lifestyle strategies for holistic care.
Medical Management
Bile acid sequestrants are particularly effective for post-cholecystectomy bile reflux. These medications bind excess bile acids and reduce gastric irritation.
Dietary Modifications
Dietary modifications become even more important after gallbladder removal. A low-fat diet helps manage continuous bile flow.
Prognosis
Most patients achieve significant symptom relief with proper medical management and dietary changes. Surgery is rarely needed.
When to Seek Immediate Medical Care
These warning signs may indicate complications requiring urgent evaluation. Contact our office immediately if you experience:
- Frequent bile vomiting (especially if it contains blood)
- Unintentional weight loss of more than 5-10 pounds
- Persistent symptoms despite treatment
- Severe or worsening upper abdominal pain
- Black or tarry stools (indicating bleeding)
- Difficulty swallowing
Frequently Asked Questions

Bile reflux can be effectively managed but may require ongoing treatment, especially if caused by permanent anatomical changes like gallbladder removal or gastric surgery. Most patients achieve significant symptom relief with bile acid sequestrants and dietary modifications. The key is consistent treatment and lifestyle adjustments.
Bile reflux involves alkaline digestive fluids (bile acids and pancreatic enzymes) rather than stomach acid. This matters because standard acid-reducing medications like antacids, H2 blockers, and PPIs don't effectively treat bile reflux. You need bile acid sequestrants and prokinetic medications specifically designed to manage bile. Many patients are frustrated after trying acid reflux treatments that don't work—proper diagnosis is crucial.
Most patients successfully manage bile reflux gastritis with medications and lifestyle changes. Surgery is reserved for severe cases that don't respond to medical treatment or when there are structural problems requiring correction. Surgical options include procedures to redirect bile flow or repair the pyloric valve.
Many patients notice improvement within 2-4 weeks of starting bile acid sequestrants and dietary modifications. Full symptom resolution may take 2-3 months. Healing of gastric inflammation (visible on endoscopy) typically requires several months of treatment. Consistency with medications and diet is essential for best results.
Expert Bile Reflux Care in Daly City
Bile reflux gastritis requires specialized knowledge and experience for accurate diagnosis and effective treatment. Many patients see multiple doctors before receiving the correct diagnosis because bile reflux is less common than acid reflux.
At Center for Diabetes and Cardiometabolic Health, our gastroenterology team has extensive experience diagnosing and treating bile reflux disorders, particularly in patients who’ve had gallbladder surgery or gastric bypass.
Meet Our Bile Reflux Treatment Specialists
Board Certified
All providers meet the highest standards of care
Same-Week Appointments
Quick access to expert care when you need it
Local to Bay Area
Serving Daly City, San Francisco & surrounding areas
- Accepting New Patients
Get Expert Treatment for Bile Reflux Gastritis
Don’t let persistent upper abdominal pain and nausea control your life. Our bile reflux specialists provide accurate diagnosis and effective treatment that addresses the root cause of your symptoms.


